The Future of Thyroid Eye Disease
- Posted on: May 6 2018
- Leave a response
Thyroid Eye disease (TED) is a disorder often associated with Graves’ disease. This autoimmune disease may attack the thyroid gland causing thyroid hormone levels to be too high or too low. The same disease may also attack the eye socket causing the eye muscles and the orbital fat to grow in size. Enlargement of the fat in the eye socket causes the eye to protrude forward. Enlargement of the eye muscles causes double vision and may also cause the eye to bulge forward. The eyelids can also be impacted and are typically too widely open, resulting in trouble closing the eyes which may in turn damage the cornea. Cigarette smoking is highly associated with the development of severe eye disease and smoking cessation is an absolute necessity to achieve the best possible outcome.
Thyroid eye disease is a spectrum of disease with some patients having so little disease that it his hardly noticeable, and some patients having severe potentially blinding disease. Vision loss in TED occurs when either the optic nerve becomes pinched by enlarging eye muscles or the cornea becomes ulcerated because the eyelids are unable to close over the protruding globe. Most commonly the thyroid hormones are high at the onset but TED may present independent of any problem with the thyroid hormones and it also may occur years after the problems with the thyroid hormones have been brought under control. Using medications to control the thyroid hormones is important to the patients overall health but does not necessarily make the eye disease any better as the underlying problem with the eye socket is not abnormal thyroid hormones but an attack of the eye socket by the immune system. So blood test can be used to support the diagnosis of TED but no hormone or antibody blood test rules out TED. Orbital imaging with CT, MRI, and ultrasound are much better at ruling out TED but in my experience they must be read and interpreted in the context of a good history and orbital examination.
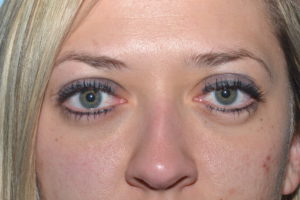
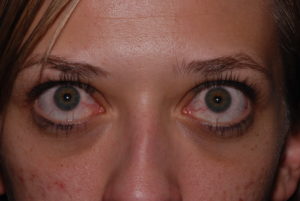
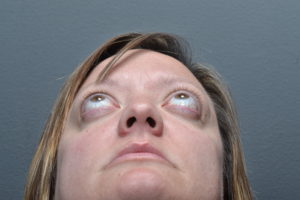
Thyroid eye disease typically has an initial period of active inflammation which damages the orbital tissues. After about a year and a half of active inflammation, the disease often enters a quiescent phase and remains quiescent in about 90% of patients. Surgery is not effective in stopping the active inflammation phase of the disease. However, once the disease becomes quiescent, eyelid surgery, orbital surgery, eye muscle surgery, and cosmetic surgery is utilized to rehabilitate the patients vision and appearance. Surgery can reverse much of the damage to both form and function and Dr. John McCann, MD has performed surgery on many patients with TED. The above photos are of a patients before and after removal of fat from the orbit which was deposited because of TED (left) and of a patient who underwent eyelid surgery to correct lid retraction caused by TED (right).
For decades the holy grail of TED treatment has been to find a safe, effective, and non-surgical treatment to turn off the disease during the active inflammatory phase so that damage to the orbital tissue never occurs. Steroids and radiation of the orbit are currently the available options for patients in the active and inflammatory phase of TED. However, these current medical treatments are not always effective and sometimes the side effects of the treatment are greater than the benefit of the treatment. Neither treatment is effective at reducing the bulging forward of the eyes caused by the disease.
A former colleague of Dr. McCann’s at UCLA, Dr. Terry Smith, and a former student of Dr. McCann’s, Dr. Raymond Douglas have been performing research for years to find a medical therapy to treat patients in the active inflammatory phase of the disease. They have recently published a clinical trial describing the benefits of a new medication called Teprotumamab in the treatment of patients with TED. Tepratumamab is a monoclonal antibody that inhibits the insulin-like growth factor receptor (IGF-IR). Studies done by Dr. Smith and Dr. Douglas in the laboratory suggested this drug may benefit patients with TED so a clinical trail was organized. A very well designed placebo controlled clinical trial published in the New England Journal of Medicine demonstrates that the drug reduces inflammation of the eye socket, double vision, and bulging forward of the eye while also improving the vision, and the appearances of patients treated during the active inflammatory phase of the disease. The side effects of the treatment were minimal. A final FDA clinal trial is underway and there is hope the drug will come to market in a couple of years.
When Teprotumamab comes to market it seems likely that doctors will finally have a better way of intervening with patients during the active and inflammatory phase of TED. In some cases Teprotumamab will prevent the disease from progressing to the point where surgical intervention is required. It is currently not known, but it seems likely, that this drug will be most effective if started during the early active inflammatory phase of the disease. The early phase of thyroid eye disease can easily be missed or misdiagnosed as conjunctivitis or dry eye. Part of the difficulty with diagnosis is that there is no blood test that definitively excludes the diagnosis of TED. Introduction of Teprotumamab will make it more important for physicians to diagnose TED in the earliest stages. This will present some diagnostic dilemmas for internist, family practice doctors, endocrinologist, and eye care professionals. Making the diagnosis of TED early before extensive damage has been done to the orbital tissues will become critical when Teprotumamab is available. Early referral of patients with suspected TED to an orbital specialist for imaging and examination will become more common when Teprotumamab becomes available.
Dr. John McCann, MD, PhD
Posted in: Blog, Center for Orbital Disease